Some Grenfell Tower survivors are scared to see a doctor
Published 23rd June 2017
By Shyamantha Asokan
Some survivors of London’s Grenfell Tower fire are scared to come forward and get the medical care they urgently need because of their immigration status, volunteer doctors at the scene say.
Grenfell Tower, a 24-storey block of flats, was destroyed in a fire last week and at least 79 deaths have been confirmed so far. Scores more people are missing and the death toll is expected to rise.
Some undocumented migrants and asylum seekers who lived at the tower are scared of getting help for fear of being referred to Home Office immigration teams, according to volunteers offering survivors medical, legal and housing support.
Dr Paquita de Zulueta, a GP who has been volunteering at a pop-up clinic for Grenfell survivors and who also volunteers at Doctors of the World’s east London clinic, spoke to the Guardian this week about this issue. She said she and her colleagues had dealt with at least three patients who were reluctant to go to hospital because of their immigration status.

De Zulueta at the Westway sports centre, which has become a hub for relief efforts and donations after the fire
De Zulueta last week saw an African woman in her early 40s who had fallen down the stairs while escaping from the tower and whose partner and relatives were missing. The woman was suffering from dizziness and memory loss, symptoms that suggested she could have a brain injury, but she didn’t want to go to A&E.
“She was frightened that she would be reported to the Home Office. I had to persuade her and reassure her, and eventually she went with an escort,” De Zulueta said.
“What we’re seeing after this fire is a particularly shocking example of something that is actually widespread – there are invisible and vulnerable people across the UK who can’t get basic and necessary healthcare,” she added.
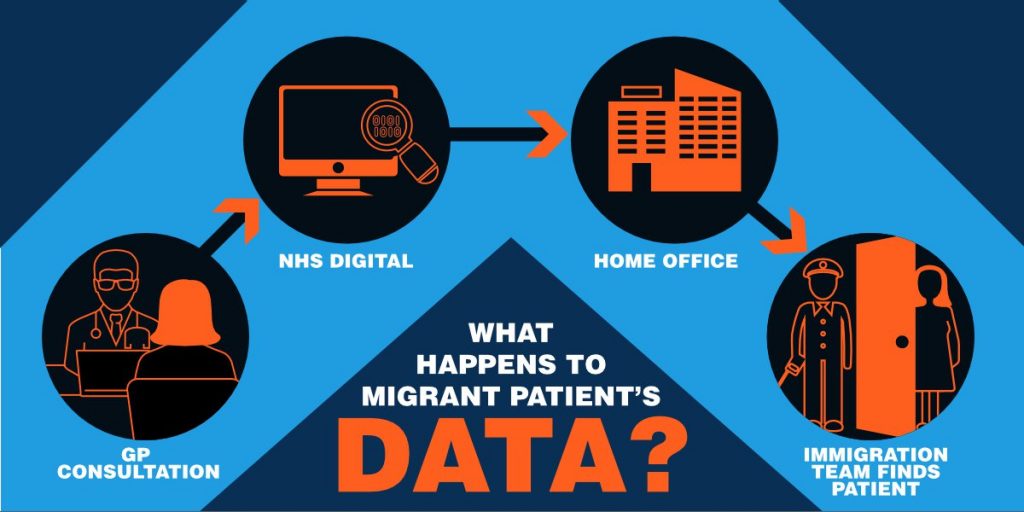
Doctors of the World’s UK clinics regularly see seriously unwell people who fear going to a doctor because of their immigration status. Home Office immigration teams can access NHS patients’ records in order to obtain private details, such as home addresses, and track down undocumented migrants.
Our #StopSharing campaign has brought together hundreds of NHS medics to stand against this data-sharing. The British Medical Association and Public Health England have also voiced serious concerns about this issue.
At Westway, a sports centre near the tower that has been converted into a relief centre, brilliant volunteer doctors and nurses are staffing a 24-hour pop-up clinic. They have helped people with psychological trauma, diabetes sufferers who lost their medication in the fire, and families who need dressings for burns.
“Things could actually get worse after a few weeks have passed,” said a nurse who did not want to be named. “That’s when the psychological impact will truly hit some people.”
Clinic volunteers have started doing outreach visits to hotels where survivors have been rehoused – there are concerns that some people are even too scared to come to Westway, where police officers are stationed at the door.
UK Prime Minister Theresa May, who has backed government moves to create a “hostile environment” for undocumented migrants for several years, said on Thursday that no immigration checks would be carried out on survivors or relatives of the dead. It’s not yet clear how much this will allay fears on the ground.
“In a situation like this, you need to remove all barriers to someone getting help,” said De Zulueta. “We’re talking about people who have lost everything – some don’t even have proper clothes anymore.”
Please help us put an end to the Home Office accessing NHS patients’ private records and making people too scared to see a doctor. Sign our #StopSharing petition.
Recent Posts
- Doctors of the World’s response to the Ebola outbreak in the DRC
- Symbolic ‘Raid’ on USAID Stockpile Containing Millions of Blocked Contraceptives
- Middle East Emergency Appeal Launched Amid Urgent Medical Needs
- War in the Middle East: Doctors of the World calls for the protection of civilians and strengthens its response to humanitarian needs
- Health, Abortion Rights, LGBTQI+ Rights, Diversity: Millions of people threatened by a U.S. Law